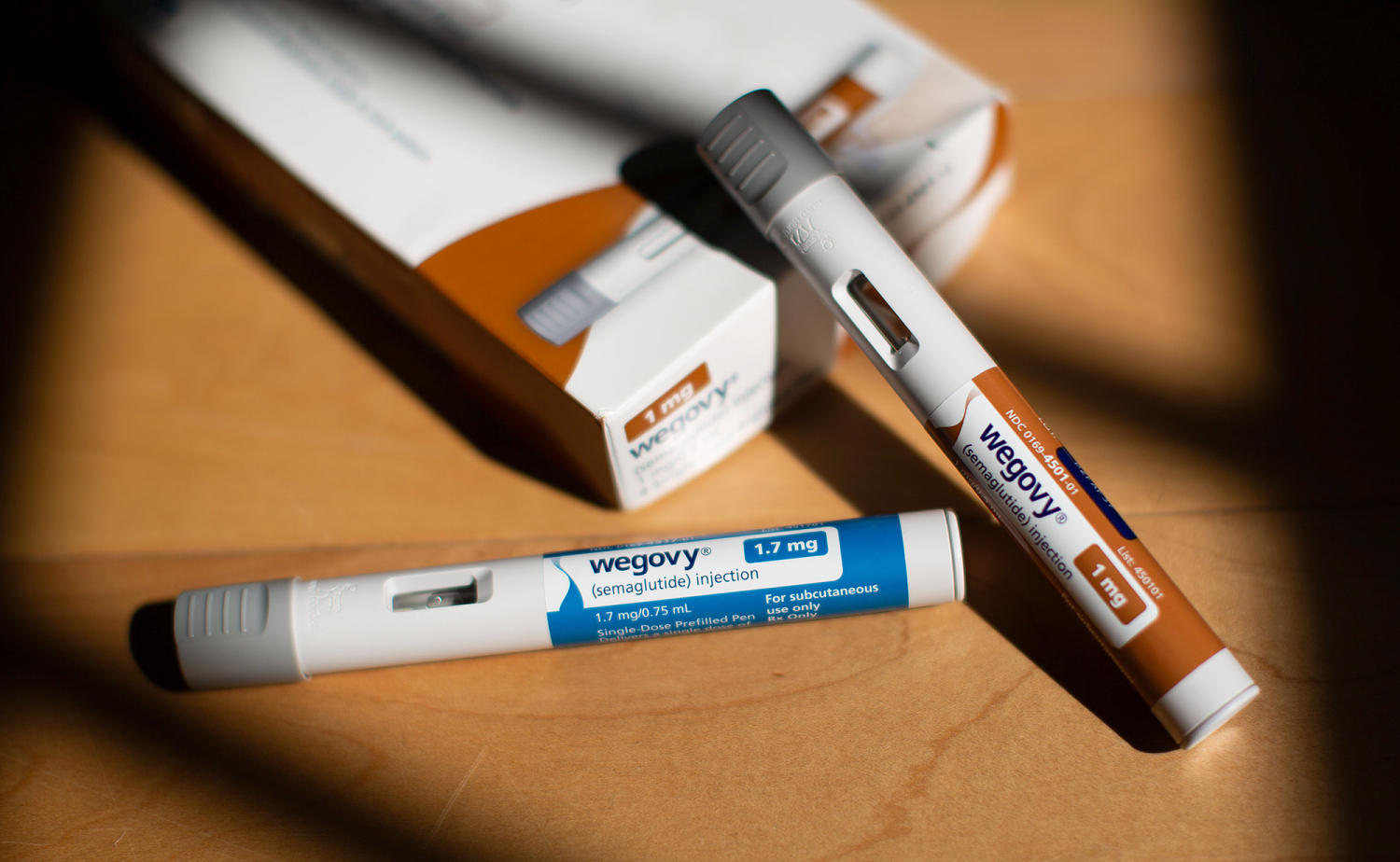
This CEO wants to cover weight loss drugs for employees. They're just too expensive.
✨ AI Summary
🔊 جاري الاستماع
Cost of DenialThis CEO wants to cover weight loss drugs for employees. They're just too expensive.As demand for GLP-1 drugs surges, employers and insurers are struggling to keep up with the cost. Some are dropping coverage altogether.Listen to this article with a free account00:0000:00Add NBC News to GoogleShould insurance cover weight loss drugs?03:23Get more newsLiveonShareAdd NBC News to GoogleApril 15, 2026, 9:24 PM EDTBy Berkeley Lovelace Jr., Jessica Herzberg and Anne ThompsonFor Dr. Joseph Cacchione, the math on GLP-1 drugs stopped making sense. Subscribe to read this story ad-free Get unlimited access to ad-free articles and exclusive content.The CEO of the Philadelphia-based nonprofit hospital system Jefferson said his organization now spends more on prescription drug coverage — fueled by the soaring use of weight loss medications like Wegovy and Zepbound — than it does on inpatient care.Jefferson has dozens of hospitals across the region. It also has its own insurance plan for its 65,000 employees. A decade ago, prescription drugs made up about 14% of Jefferson’s insurance spending, Cacchione said. Last year, it was 40%. In 2025, Jefferson’s insurance arm reported about a $180 million loss, about a third of which was driven by coverage of GLP-1s, the CEO said. He was forced to lay off more than 600 employees as drug coverage ate up operating costs. This year, the insurance plan started requiring employees to go through diet and lifestyle programs before it would cover GLP-1 drugs for weight loss — a restriction Cacchione said has already saved Jefferson $20 million. “We understand the value of them, but they are putting a big stress on the system,” he said. “The system wants to pay for them. We just can’t afford to pay for them right now.”More from NBC News' Cost of Denial seriesA liver transplant might save him — if he can get the drug he needs to stay alive long enoughHer spine surgery was denied. Doctors say it’s all too common.Patients hit de...





